Headaches
Osteopathic Management for Headaches — Melbourne & Caroline Springs
Headaches are a common health concern that can significantly affect comfort, concentration, and daily function.
At Live Well Health Centre, osteopaths help assess and manage certain types of headaches, particularly those influenced by the neck, muscles, posture, and movement patterns.
Our approach focuses on understanding contributing factors, improving function, and supporting long-term symptom management.
What are headaches?
A headache is pain or discomfort felt in the head, scalp, or upper neck region.
There are many different types of headaches. Some are primarily neurological, while others are influenced by musculoskeletal factors.
Osteopathic care commonly focuses on headaches that involve mechanical or movement-related contributors, including:
- cervicogenic headaches (originating from the neck)
- tension-type headaches
- headaches associated with posture or muscle tension
Some people with migraine may also have musculoskeletal contributors that influence symptom frequency or severity, although migraines are a complex neurological condition requiring medical management.
Common symptoms
Headache symptoms vary depending on type but may include:
- aching, pressure, or tightness around the head
- pain starting in the neck and spreading to the head
- reduced neck movement
- tenderness in neck or shoulder muscles
- headaches triggered by posture or movement
Some individuals may experience:
- light or sound sensitivity
- nausea
- visual disturbance (in some headache types)
Severe, sudden, or unusual headaches require urgent medical assessment.

What causes headaches?
Headaches often have multiple contributing factors.
Common musculoskeletal contributors include:
- neck joint dysfunction
- muscle tension in the neck or shoulders
- prolonged or sustained posture
- reduced movement variability
- stress-related muscle activation
- jaw tension or TMJ dysfunction
Other factors may include:
- sleep disturbance
- fatigue
- dehydration
- neurological or vascular mechanisms (in migraine and other headache disorders)
Not all headaches are musculoskeletal, which is why proper assessment is important.
Who is most likely to experience headaches?
Headaches can affect people of all ages.
They are commonly seen in:
- desk-based workers
- people with sustained posture demands
- individuals experiencing stress or muscle tension
- people with neck pain or restricted movement
- individuals with jaw tension or clenching
- those with previous neck injury
How are headaches assessed?
Osteopathic assessment may include:
- detailed symptom history
- headache pattern and triggers
- neck movement assessment
- muscle and joint examination
- posture and functional movement evaluation
Because some headaches require medical management, referral to a GP or specialist may be recommended if symptoms suggest a non-musculoskeletal cause.
How osteopathy may help manage headaches
Osteopaths help manage headaches by addressing mechanical and functional factors that may contribute to symptoms.
Management may involve:
- improving neck mobility
- reducing muscle tension
- supporting posture and movement
- addressing contributing jaw or shoulder dysfunction
- providing movement and self-management strategies
Care is individualised and may include education, rehabilitation, and lifestyle guidance.
Osteopathic management is commonly part of a broader healthcare approach and may occur alongside GP or specialist care when appropriate.
Techniques that may be used
Depending on assessment findings, management may include:
- joint mobilisation of the neck and upper spine
- soft tissue techniques
- muscle energy technique (MET)
- postural and movement retraining
- exercise rehabilitation
- clinical Pilates
- TMJ management where relevant
Technique selection depends on individual presentation and clinical reasoning.
Evidence and research
Clinical guidelines support conservative, non-pharmacological approaches for certain headache types, particularly tension-type and cervicogenic headaches.
Evidence supports:
- manual therapy combined with exercise
- physical therapy for neck-related headaches
- multimodal management including education and movement
Key guideline and research sources
International Headache Society — Classification of Headache Disorders
Recognises cervicogenic headache as a secondary headache originating from cervical structures.
Jull et al., Randomised Controlled Trials — Cervicogenic Headache
Demonstrated benefit from targeted physical therapy including manual therapy and exercise.
Gross et al., Cochrane Reviews — Manual Therapy for Headache
Suggest manual therapy may improve pain and function in cervicogenic headache when combined with exercise.
European Federation of Neurological Societies Guidelines
Support physical therapy approaches for cervicogenic headache management.
Clinical interpretation
Multimodal care that includes movement, education, and musculoskeletal management is widely recommended for headaches with mechanical contributors.
What to expect from management
Management plans depend on:
- headache type
- symptom duration
- contributing factors
- individual goals
Some people experience gradual improvement as movement and contributing factors are addressed.
Active participation — including movement strategies and rehabilitation — is often an important part of management.
Self-management and lifestyle support
Education and behaviour strategies are often part of headache management.
Your osteopath may guide:
- posture and workstation setup
- movement breaks
- neck mobility exercises
- stress and muscle tension awareness
- load management
When to seek medical review
Urgent medical assessment is required if headaches involve:
- sudden severe onset (“worst headache ever”)
- neurological symptoms
- visual loss
- confusion or altered consciousness
- fever or systemic illness
- headache following trauma
If unsure, seek medical advice.
Frequently asked questions
Can neck problems cause headaches?
Yes. Some headaches originate from cervical spine dysfunction.
Can osteopathy help migraines?
Osteopathy does not treat migraine itself but may help manage musculoskeletal factors that contribute to symptoms in some people.
Do I need imaging for headaches?
Imaging is not routinely required unless clinical indicators suggest further investigation.
Is shockwave therapy covered by Medicare or private health?
Stress can influence muscle tension, which may contribute to some headache types.
Related conditions
- Neck pain
- TMJ dysfunction
- Postural strain
- Upper back pain
Not sure what type of headache you have?
If you are unsure what is causing your headaches, an osteopathic assessment can help identify contributing factors and guide appropriate management.
Book an appointment to discuss your symptoms.
Have you ever experienced a headache? If so, you comprehend the sheer debilitation it can bring.
Recent research by ‘Headache and Migraine Australia’ unveiled that within the past year, 4.9 million Australians endured headaches or migraines. Astonishingly, 60% of these sufferers underwent reduced social interactions and noted a decline in work efficiency (1).
The ‘World Health Organisation’ classifies headaches as nervous system conditions, with head pain merely one of several symptoms (2). Headaches fall into two categories: Primary; arising without an underlying medical condition, often triggered by lifestyle factors, sleep issues, or diet (2,3). Secondary; stemming from medical causes like sinus congestion, eye strain, and dental problems (2,3).
Managing a secondary headache involves treating underlying medical causes. However, Osteopathy predominantly addresses primary headaches. Research identifies the upper cervical spine’s role in headaches and migraines (4). Migraine and Tension Type Headache are the prevalent primary headaches seen in Osteopathy.
While stress might play a role, musculoskeletal neck conditions such as poor posture, prolonged desk work, or challenging sleep patterns are more commonly associated with these headaches.
Let’s delve into the world of migraines:
These neurological disorders induce moderate to severe head pain, often characterised as a pulsating sensation on one side of the head. In addition to head pain, migraines can bring about various symptoms like nausea, vomiting, dizziness, visual alterations, and even numbness and tingling in the face (2,3).
Interestingly, migraines tend to debut during puberty and persist throughout life. Women are more susceptible to these headaches, with hormonal shifts during menstruation, menopause, and pregnancy believed to play a role (2).
Migraine attacks can strike unpredictably, ranging from multiple occurrences weekly to just once a year. Surprisingly, the precise triggers behind these attacks remain elusive.
Transitioning to tension type headaches:
A substantial 70% of the population grapples with this, which are often characterised as a dull ache accompanied by a sensation of tightness around the head (2,3). Typically, the pain associated with tension type headaches falls within the mild to moderate range.
They generally occur in episodes, lasting anywhere from a few hours to several days (2,3). For some, chronic tension headaches persist for up to 15 days each month (2).
While stress may contribute to their occurrence, tension type headaches are more commonly associated with musculoskeletal conditions in the neck. Factors like poor posture, extended desk hours, and even challenging sleep patterns can amplify their presence.
Unlocking the Benefits of Osteopathy:
Wondering how Osteopathy can be your solution? Osteopaths possess the expertise to diagnose and address various headache types. They’re also adept at recognising any worrisome symptoms that might warrant consultation with your GP or neurologist.
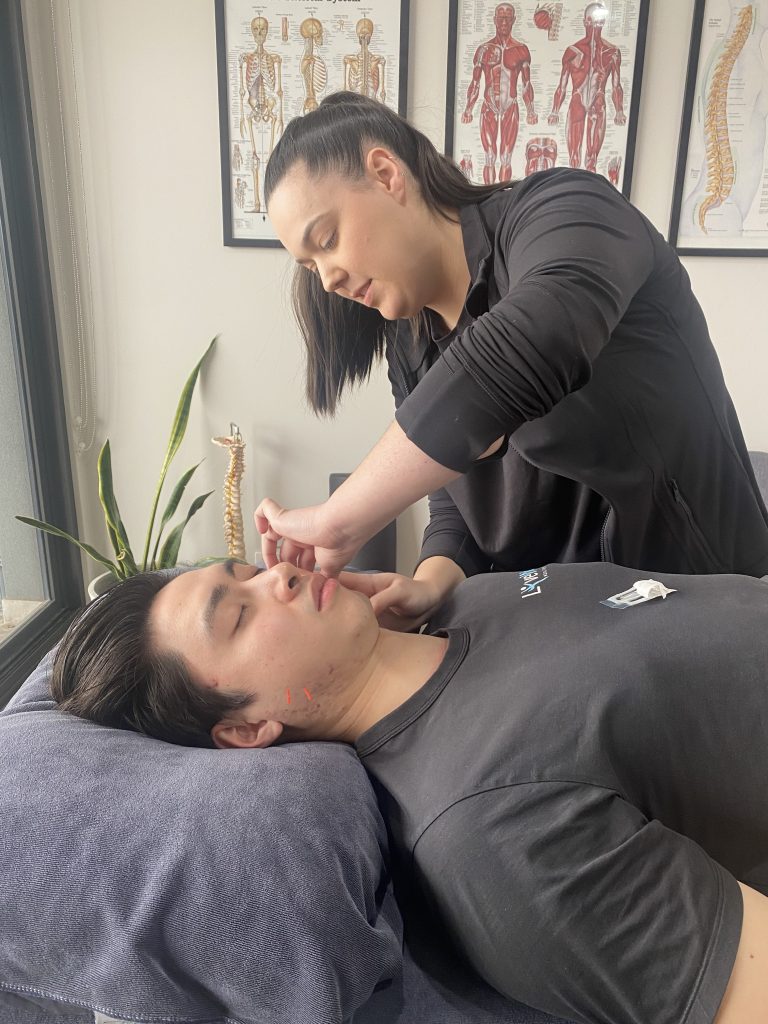
Using a multifaceted approach, Osteopathy leverages a range of techniques for targeted relief. These include soft tissue massage, joint mobilisation, manipulation, strategic dry needling, and targeted strength-based exercises. This holistic approach is designed to help curtail the occurrence of both headaches and migraines, providing you with longer lasting relief.
Ready to experience the impact of Osteopathy? Our team at LWHC is here to guide you toward a life with fewer headaches and enhanced well-being.
References
(1) Why Does My Shoulder Hurt? [Internet]. Healthline. 2020 [cited 28 August 2020]. Available from: https://www.healthline.com/health/chronic-pain/shoulder-pain
(2) HILL C, GILL T, SHANAHAN E, TAYLOR A. Prevalence and correlates of shoulder pain and stiffness in a population-based study: the North West Adelaide Health Study. International Journal of Rheumatic Diseases. 2010;13(3):215-222.
(3) Ackerman I, Page R, Fotis K, Schoch P, Broughton N, Brennan-Olsen S et al. Exploring the personal burden of shoulder pain among younger people in Australia: protocol for a multicentre cohort study. BMJ Open. 2018;8(7).
(4) Shoulder Pain and Common Shoulder Problems – OrthoInfo – AAOS [Internet]. Orthoinfo.aaos.org. 2020 [cited 28 August 2020]. Available from: https://orthoinfo.aaos.org/en/diseases–conditions/shoulder-pain-and-common-shoulder-problems/
(5) 1. Wilson C. [Internet]. 2015 [cited 28 August 2020]. Available from: https://www.shoulder-pain-explained.com/shoulder-pain-causes.html
(6) Frost A, Michael Robinson C. The painful shoulder. Surgery (Oxford). 2006;24(11):363-367.
(7) Shoulder Instability [Internet]. 2020 [cited 28 August 2020]. Available from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/shoulder-instability
(8) Shoulder Arthritis [Internet]. 2020 [cited 28 August 2020]. Available from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/shoulder-arthritis
(9) Nordqvist A, Petersson C. Incidence and causes of shoulder girdle injuries in an urban population. Journal of Shoulder and Elbow Surgery. 1995;4(2):107-112.
(10) Brian Subach M. Could That Shoulder Pain Really Stem From the Neck? [Internet]. Spine-health. 2020 [cited 28 August 2020]. Available from: https://www.spine-health.com/conditions/neck-pain/could-shoulder-pain-really-stem-neck

Dr Samantha Volarich
Osteopath
Watson Headache and Migraine Institute
