Benign Paroxysmal Positional Vertigo (BPPV)
Osteopathic Assessment & Supportive Management — Melbourne & Caroline Springs
Benign paroxysmal positional vertigo (BPPV) is a common cause of brief episodes of dizziness or spinning sensations triggered by changes in head position.
At Live Well Health Centre, our osteopaths provide assessment and evidence-informed supportive management for people experiencing symptoms consistent with BPPV. Care focuses on identifying positional triggers, supporting safe movement, and guiding appropriate management strategies.
Management is individualised and may be provided alongside care from your GP or other medical professionals where appropriate.
What is BPPV?
BPPV is a vestibular (inner ear) condition that can cause short episodes of vertigo — a sensation that the room is spinning or moving.
It occurs when tiny calcium crystals (otoconia) inside the inner ear become displaced and move into areas where they disrupt normal balance signalling.
Symptoms are typically triggered by changes in head position, such as:
- rolling in bed
- looking up or down
- bending forward
- getting in or out of bed
Episodes are usually brief but may be unsettling.
Common symptoms
BPPV may cause:
- brief spinning sensations with head movement
- dizziness when changing position
- loss of balance or unsteadiness
- nausea during episodes
- symptoms when turning in bed
- sensitivity to rapid head movement
Symptoms usually occur in short bursts and may resolve between episodes.
BPPV does not typically cause constant dizziness, hearing loss, or neurological symptoms.
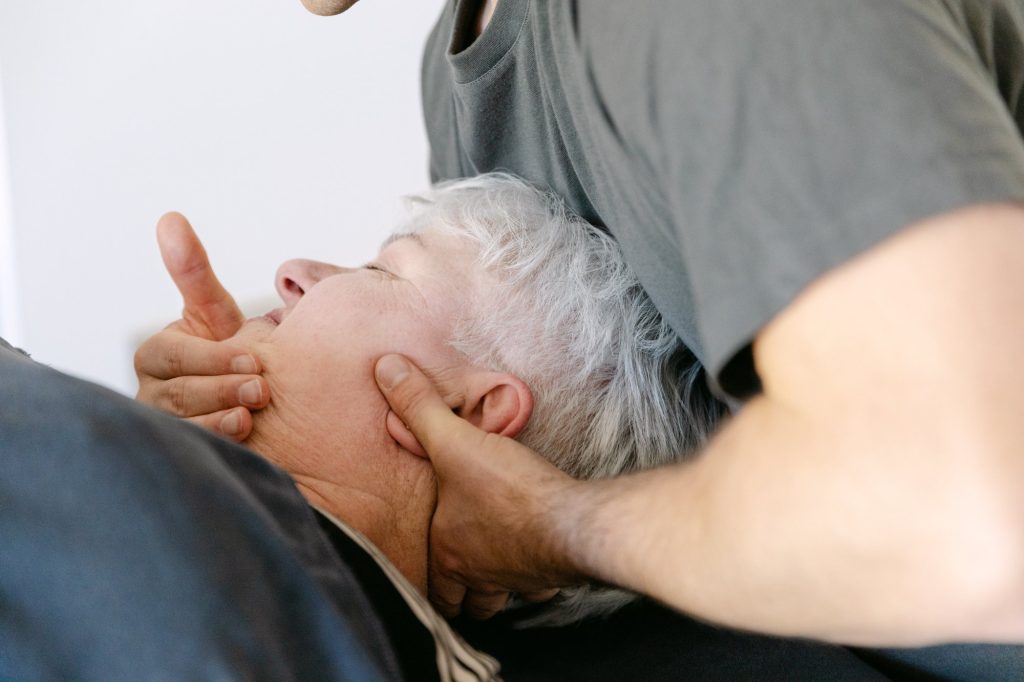
Why BPPV can occur
BPPV can develop when inner ear crystals become displaced. This may occur:
- without a clear cause (common)
- after head movement or minor trauma
- following illness affecting the inner ear
- with age-related inner ear changes
- after prolonged bed rest
Many people experience a sudden onset without an obvious trigger.
Who is more likely to experience BPPV?
BPPV is more common in:
- adults over 40
- people with a history of vertigo
- those who have experienced head injury
- individuals with inner ear conditions
- people who have recently been unwell or inactive
However, it can occur at any age.
Osteopathic assessment for suspected BPPV
Assessment focuses on identifying whether symptoms are consistent with positional vertigo and determining appropriate management.
This may include:
- detailed symptom history
- identification of positional triggers
- observation of eye movement responses (where appropriate)
- balance and movement assessment
- screening for non-vestibular causes of dizziness
If symptoms suggest another cause of vertigo or require medical investigation, referral to your GP or specialist will be recommended.
Osteopathic care does not replace medical diagnosis.
How osteopathy may support management of BPPV
Osteopathic management aims to support safe movement and symptom management. This may involve:
- identifying and guiding positional movement strategies
- supporting neck comfort during positional changes
- providing education about symptom triggers
- helping restore confidence with movement
- guiding gradual return to usual activity
Where appropriate and clinically indicated, repositioning manoeuvres may be used to assist movement of inner ear crystals.
Management is individualised and based on clinical findings.
Approaches that may be used
Depending on assessment findings, care may include:
- positional assessment and guidance
- canalith repositioning manoeuvres (when appropriate)
- balance and movement support
- education on symptom management
- gradual movement re-exposure strategies
- neck mobility support where required
Care is adapted to symptom sensitivity and safety.
Evidence and clinical guidelines
BPPV is widely recognised in clinical guidelines, with positional assessment and repositioning manoeuvres commonly recommended as first-line management where appropriate.
Key evidence sources:
American Academy of Otolaryngology — Head and Neck Surgery (AAO-HNS)
Clinical practice guideline: benign paroxysmal positional vertigo
National Institute for Health and Care Excellence (NICE)
Vertigo and vestibular disorder guidance
Cochrane Review — Repositioning manoeuvres for BPPV
Vestibular Disorders Association (VeDA)
Patient information on BPPV
These sources support positional assessment and movement-based management for many cases of BPPV.
What to expect from management
Experiences vary between individuals. Symptom change may depend on:
- duration of symptoms
- specific canal involvement
- sensitivity to movement
- adherence to movement guidance
Some people experience rapid improvement, while others require gradual adaptation.
Self-management strategies your osteopath may discuss
- safe movement strategies during episodes
- sleeping position guidance
- pacing head movements
- gradual return to normal activity
- balance confidence strategies
When to seek urgent medical review
Seek immediate medical attention if dizziness occurs with:
- severe headache
- double vision
- slurred speech
- weakness or numbness
- difficulty walking
- chest pain
- fainting or loss of consciousness
These symptoms are not typical of BPPV and require urgent assessment.
Frequently asked questions
Is BPPV dangerous?
BPPV is usually not serious, but proper assessment is important to confirm the cause of vertigo.
Can BPPV return?
Some people experience recurrence. Assessment helps guide appropriate management if symptoms return.
Is osteopathy a replacement for medical care?
No. Osteopathic care is supportive and may be used alongside medical assessment and management.
Related conditions
- Vertigo
- Vestibular dysfunction
- Neck pain
- Balance disorders
- Cervicogenic dizziness
Book an assessment
If you are experiencing dizziness or spinning sensations triggered by movement, our osteopaths can assess your symptoms and discuss appropriate supportive management.
Book an appointment to discuss your BPPV symptoms.
Health information disclaimer
This information is general education and is not a substitute for personalised medical advice. Individual assessment is required to determine appropriate care. Diagnosis and medical management should be guided by a qualified health professional.

