Myofascial Pain
Osteopathic Management for Muscle & Fascial Pain — Melbourne & Caroline Springs
Myofascial pain is a common cause of persistent muscle discomfort, tightness, and referred pain patterns that can affect movement and daily function.
At Live Well Health Centre, osteopaths help assess and manage myofascial pain by identifying areas of muscle and connective tissue tension and addressing the movement and load patterns contributing to symptoms.
Our approach focuses on restoring normal muscle function, improving movement quality, and supporting long-term symptom management.
What is myofascial pain?
Myofascial pain refers to pain arising from muscles and fascia — the connective tissue that surrounds and supports muscles throughout the body.
It is commonly associated with:
- muscle tightness
- trigger points (sensitive spots within muscle)
- referred pain patterns
- restricted movement
Fascia plays an important role in force transmission and movement coordination. When muscles or fascia become overloaded, irritated, or sensitised, pain and stiffness may develop.
Myofascial pain may be localised or spread across broader areas of the body.
Common symptoms
Myofascial pain may involve:
- deep aching muscle pain
- tight or tender muscle bands
- pain that spreads to other areas (referred pain)
- reduced range of movement
muscle stiffness - fatigue in affected muscles
- sensitivity when pressure is applied
Symptoms often persist or fluctuate rather than appearing suddenly after injury.
What causes myofascial pain?
Myofascial pain often develops when muscles or connective tissues are exposed to prolonged or repeated stress.
Common contributing factors include:
- repetitive movement
- sustained postures (e.g. desk work)
- muscle overload
- stress-related muscle tension
- previous injury
- reduced physical activity
- movement imbalance
Pain may persist if underlying load or movement patterns are not addressed.
Who is most likely to experience myofascial pain?
Myofascial pain is commonly seen in:
- desk-based workers
- people under prolonged physical or emotional stress
- individuals with repetitive work tasks
- athletes or active individuals
- people with chronic musculoskeletal pain
- individuals with postural strain
It can affect people of all ages.
How is myofascial pain assessed?
Osteopathic assessment typically includes:
- detailed symptom history
- movement assessment
- muscle palpation
- identification of tender or trigger point areas
- posture evaluation
- load and activity assessment
Assessment focuses on identifying contributing movement and tissue factors.
Referral to a GP or specialist may be advised if clinically indicated.
How osteopathy may help manage myofascial pain
Osteopaths help manage myofascial pain by addressing muscle function, movement patterns, and tissue loading.
Management may involve:
- reducing muscle tension
- improving movement and mobility
- restoring load tolerance
- improving posture and movement habits
- guiding strengthening and rehabilitation
Care is individualised and often includes active rehabilitation strategies.
Techniques that may be used
Based on assessment findings, management may include:
- soft tissue techniques
- myofascial release
- trigger point therapy
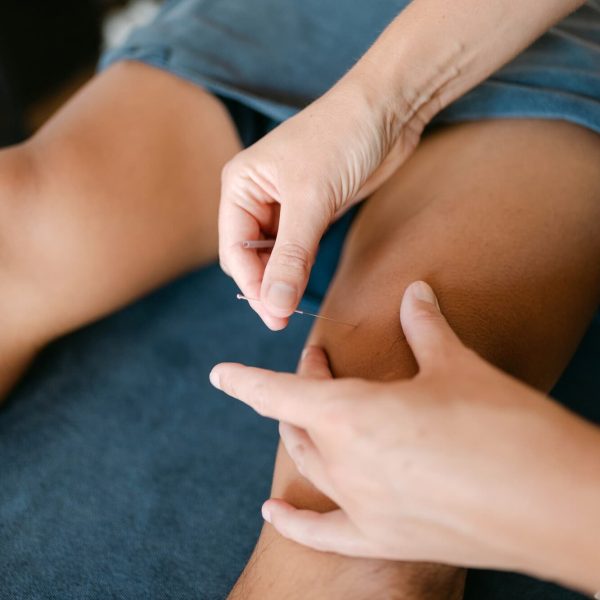
- dry needling
- muscle energy technique (MET)
- movement retraining
- exercise prescription
- clinical Pilates
Technique selection depends on clinical reasoning and patient presentation.
Evidence & research
Research supports multimodal management for myofascial pain, including manual therapy, movement-based rehabilitation, and education.
Evidence suggests:
- manual therapy may reduce pain sensitivity short term
- exercise improves muscle function and movement control
- trigger point treatment may reduce local muscle tenderness
- combined approaches are typically most effective
Key evidence sources
StatPearls — Myofascial Pain Syndrome
https://www.ncbi.nlm.nih.gov/books/NBK499882/
Journal of Bodywork and Movement Therapies — Myofascial Pain Research
https://www.sciencedirect.com/journal/journal-of-bodywork-and-movement-therapies
British Journal of Sports Medicine — Soft Tissue Pain Management
https://bjsm.bmj.com
American Academy of Family Physicians — Trigger Points and Myofascial Pain
https://www.aafp.org/pubs/afp/issues/2002/0215/p653.html
Clinical interpretation
Management approaches combining manual therapy, movement rehabilitation, and education are widely recommended for persistent muscle and fascial pain.
What to expect from management
Recovery depends on:
- duration of symptoms
- contributing movement patterns
- tissue sensitivity
- rehabilitation consistency
Many people experience improvement when both local muscle tension and broader movement patterns are addressed.
Self-management and lifestyle support
Your osteopath may guide:
- movement and posture strategies
- strengthening exercises
- stress management approaches
- activity pacing
- regular movement breaks
Consistency supports long-term symptom management.
When to seek medical review
Medical assessment is recommended if symptoms include:
- unexplained widespread pain
- significant neurological symptoms
- persistent symptoms despite management
- systemic or non-mechanical symptoms
If unsure, seek medical advice.
Frequently asked questions
Is myofascial pain the same as muscle tightness?
Not always. It involves both muscle and connective tissue sensitivity and may include referred pain.
Are trigger points real?
Trigger points are widely described clinically as tender areas within muscle associated with pain and sensitivity.
Will massage alone fix it?
Manual therapy may help symptoms, but movement and rehabilitation are usually important for long-term management.
Is myofascial pain chronic?
It can become persistent if contributing factors are not addressed.
Related conditions
- Neck pain
- Back pain
- Postural strain
- Headaches
Not sure if your pain is myofascial?
If you are experiencing persistent muscle tightness, tenderness, or referred pain patterns, an osteopathic assessment can help identify contributing factors and guide appropriate management.
Book an appointment to discuss your symptoms.

